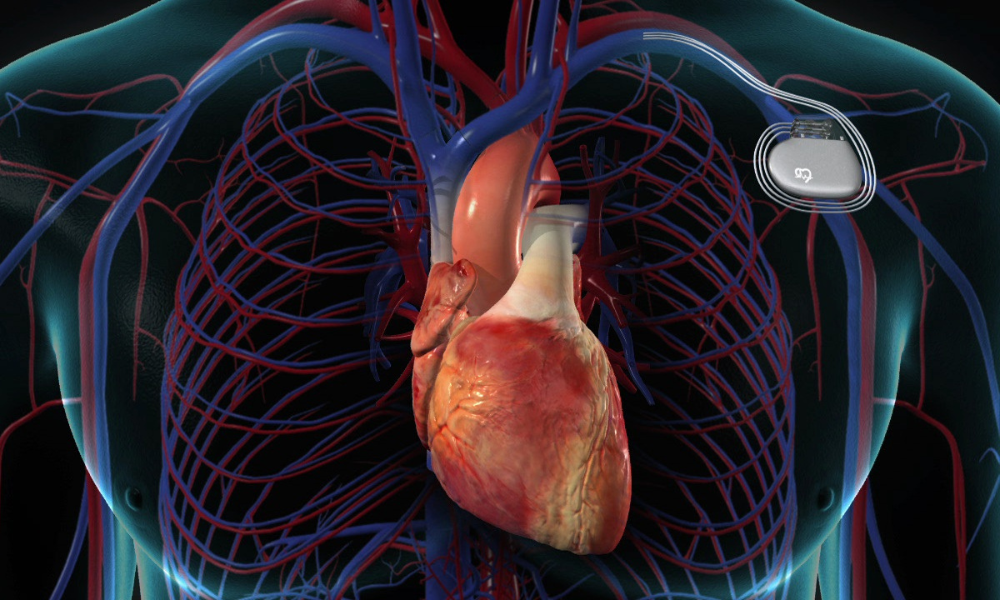
Pacemaker implantation is a minimally invasive cardiac procedure designed to treat heart rhythm disorders (arrhythmias) such as bradycardia (slow heart rate) or irregular heartbeats. The pacemaker is a small electronic device placed under the skin in the chest that helps the heart maintain a normal rhythm and ensures efficient blood circulation.
Types of Pacemakers
- 1. Single-Chamber Pacemaker – Contains one lead that is placed in either the right atrium or the right ventricle to regulate the heartbeat.
- 2. Dual-Chamber Pacemaker – Has two leads, one in the right atrium and one in the right ventricle, helping coordinate timing between the upper and lower chambers of the heart.
- 3. Biventricular Pacemaker (CRT Device) – Includes three leads placed in the right atrium, right ventricle, and left ventricle. It is used for cardiac resynchronization therapy (CRT) in patients with heart failure to improve heart pumping efficiency.
Preparation
- Evaluation: Pre-procedure assessments such as ECG, echocardiogram, and blood tests are performed to evaluate the patient’s heart condition.
- Medication: Certain medications, particularly blood thinners, may be temporarily stopped prior to the procedure.
- Fasting: Patients are generally asked to fast for several hours before surgery.
Implantation Procedure
- Anesthesia: The procedure is performed under local anesthesia with mild sedation to keep the patient comfortable.
- Incision: A small incision (usually below the collarbone) is made.
- Lead Placement: One or more leads (wires) are inserted through a vein and guided into the heart chambers using fluoroscopic (X-ray) guidance.
- Device Placement: The pacemaker generator is placed in a pocket under the skin near the incision site.
- Testing & Programming: The leads are connected to the device and tested to ensure correct pacing. The pacemaker is then programmed to match the patient’s specific heart rhythm needs.
- Closure: The incision is closed using sutures or surgical glue.
Post-Procedure Care
- Monitoring: The patient is monitored for several hours or overnight for any complications such as bleeding, swelling, or lead displacement.
- Programming: The pacemaker’s settings are fine-tuned for optimal performance.
- Medications: Patients may be prescribed antibiotics to prevent infection and given guidance on resuming regular medicines.
- Activity Restrictions: Patients are advised to avoid lifting heavy objects or raising the arm on the implantation side for a few weeks.
Advantages of Pacemaker Implantation
- Relief from Symptoms: Reduces dizziness, fainting, and fatigue caused by irregular or slow heartbeats.
- Improved Heart Function: Helps maintain a stable and effective heartbeat, improving oxygen delivery to the body.
- Enhanced Quality of Life: Enables patients to resume normal activities with better energy levels and stamina.
- Durability: Modern pacemakers last 5 to 15 years, depending on device type and usage.
Leadless Pacemaker
Next-Generation, Minimally Invasive Pacemaker Technology
This technology offers improved safety, fewer complications, and better comfort — especially for patients requiring long-term pacing.
Who Needs a Leadless Pacemaker?
Leadless Pacemakers are used in patients with:
- Symptomatic bradycardia
- Atrial fibrillation with slow ventricular response
- Sick sinus syndrome
- Atrioventricular (AV) block (selected cases)
- Patients with high risk of infection (diabetes, CKD, immunocompromised)
They are especially preferred for:
- Patients with previous pacemaker infections
- Elderly and frail patients
- Those with limited venous access or venous occlusion
- Patients undergoing hemodialysis
- Patients who wish to avoid visible scars or leads
How Is the Procedure Performed?
- Local anesthesia and light sedation are administered
- A catheter is inserted through the femoral vein
- The device is guided into the right ventricle
- It is secured to the heart tissue using soft tines or screws
- Device function is tested and confirmed
- The catheter is removed and the puncture site is sealed — no sutures needed
Safety & Outcomes (Guideline and Study Data)
According to global trials (Micra IDE, Micra Coverage with Evidence Development, Aveir DR trials):
- 98–99% implantation success
- ~50–90% reduction in infection and lead-related complications
- Excellent long-term pacing stability
Indian tertiary EP centres report outcomes comparable to global standards, with rising adoption, especially in patients with high infection risk or dialysis access considerations.

Dr. Ritesh Acharya
Cardiologist Electrophysiologist
10:00 AM – 08:00 PM
Bhubaneswar, Odisha
📞 9438181786
✉️ acharyaritesh1987@gmail.com
Doctor Details
Qualifications:
M.B.B.S., M.D. (General Medicine), D.M. (Cardiology),
Post D.M. Fellowship in Cardiac Electrophysiology and Device Therapy
Current Position:
Consultant Cardiologist & Electrophysiologist
Hi-Tech Medical College & Hospital, Bhubaneswar
Experience:
• Consultant Cardiologist & Electrophysiologist – Hi-Tech Medical College & Hospital (Sept 2025 – Present)
• Sunshine Hospital, Bhubaneswar (Mar 2024 – Sept 2025)
• Medicover Hospital, Hyderabad – Post Doctoral Fellowship (2023–2024)
• KIMS, Bhubaneswar – Assistant Professor & Senior Resident (2021–2022)
Areas of Specialisation
- Electrophysiology study & RF ablation (2D & 3D mapping)
- Dual chamber pacemaker & ICD implantation
- Coronary angiogram & angioplasty
- Peripheral angiogram & pericardiocentesis
- Conduction system pacing & CRT implantation
- PTMC, TAVI, ASD, VSD & PDA closure
- 2D & Colour Doppler Echocardiography
Biodata
Dr. Ritesh Acharya is a highly trained Cardiologist and Electrophysiologist with extensive experience in advanced cardiac electrophysiology, device therapy, and coronary interventions.
His academic background includes training at SCB Medical College, KIMS Bhubaneswar, and a Post Doctoral Fellowship in Cardiac Electrophysiology from Medicover Hospital, Hyderabad.
He has multiple national and international publications including articles in New England Journal of Medicine, Indian Heart Journal, and CSI Update. He is an active participant and presenter at IHRS, CSI, and APICON conferences.
Place: Bhubaneswar