Valvular Heart Disease
Valvular heart disease (VHD) refers to any disorder that affects one or more of the heart’s valves — mitral, aortic, tricuspid, or pulmonary. These valves ensure one-way blood flow through the heart chambers. When damaged or diseased, they may not open or close properly, disrupting normal blood circulation. VHD can be congenital (present at birth) or acquired due to infections, age-related degeneration, or other heart conditions.
Coronary angiography and angioplasty
Renal Angioplasty
Coronary Angiography
Left Main Angioplasty
Pre-Procedure Assessment
Calcified Arteries
Pacemaker Implantation
Valvular Heart Disease
Endovascular Graft Repair
Device Closures
Peripheral Interventions
Renal Angioplasty
Non Invasive Cardiology
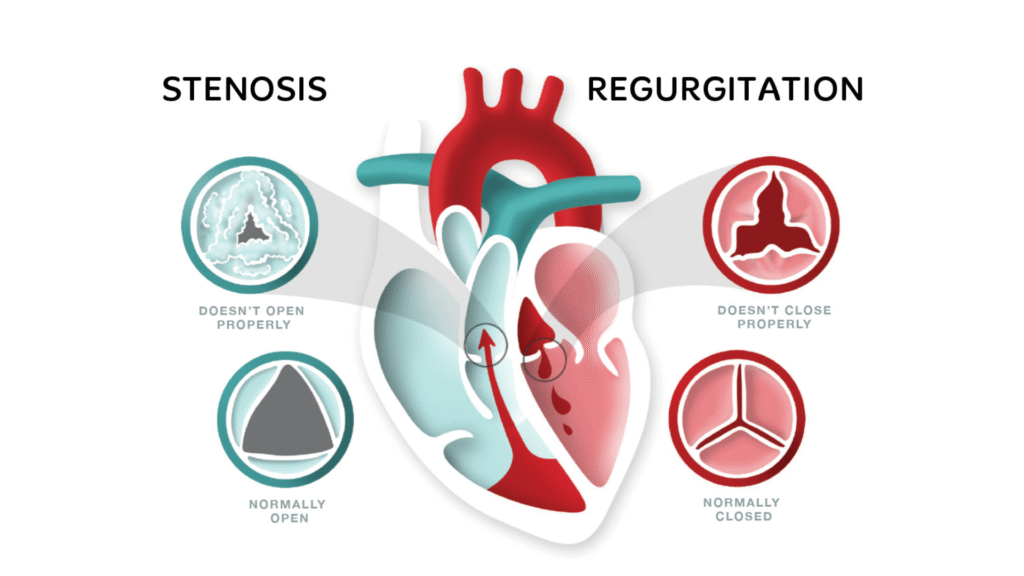
Types of Valvular Heart Disease
Stenosis: The valve does not open fully, restricting blood flow.
Regurgitation (Insufficiency): The valve does not close completely, causing blood to leak backward.
Atresia: The valve lacks an opening for blood to pass through (usually congenital).
Symptoms
Shortness of Breath: Especially noticeable during physical activity or when lying flat.
Fatigue and Weakness: Due to reduced blood flow and oxygen delivery.
Palpitations: Sensation of fluttering or irregular heartbeat.
Chest Pain or Pressure: Common in aortic stenosis.
Swelling (Edema): In the legs, ankles, or abdomen due to fluid buildup.
Dizziness or Fainting: Especially during exertion, often linked with severe aortic stenosis.
Diagnosis
Physical Examination: Detection of heart murmurs and abnormal heart sounds using a stethoscope.
Echocardiography: Key diagnostic test to assess valve structure and function.
Transthoracic Echocardiography (TTE): Non-invasive imaging from the chest wall.
Transesophageal Echocardiography (TEE): Provides detailed valve images through the esophagus.
Electrocardiogram (ECG): Evaluates the heart’s electrical activity and rhythm disturbances.
Chest X-ray: Shows heart enlargement and signs of fluid in the lungs.
Cardiac MRI: Offers high-resolution imaging of valve anatomy and function.
Cardiac Catheterization: Measures pressure in heart chambers and confirms the severity of valve disease.
Treatment
1. Medications
Diuretics: Help reduce fluid buildup in the lungs and body.
Beta-Blockers: Control heart rate and lower blood pressure.
ACE Inhibitors / ARBs: Reduce heart workload and improve blood flow.
Anticoagulants: Prevent blood clots in conditions like atrial fibrillation associated with VHD.
2. Interventional Procedures
Balloon Valvuloplasty: A minimally invasive procedure to widen a narrowed valve (mainly used for mitral or aortic stenosis).
Transcatheter Aortic Valve Replacement (TAVR): A less invasive alternative to open-heart surgery for aortic valve replacement.
3. Surgical Options
Valve Repair: Preferred for preserving the patient’s own valve, especially in the mitral or tricuspid position.
Valve Replacement: Involves implanting either a mechanical or biological (tissue) valve when repair isn’t possible.
Post-Treatment Care
Regular follow-up visits with echocardiography to monitor valve function.
Lifestyle Modifications:
Heart-healthy diet (low sodium, low fat).
Regular, moderate exercise.
Avoid smoking and limit alcohol intake.
Medication Adherence: Especially for patients with mechanical valves who require lifelong anticoagulation.
Prognosis and Prevention
Prompt treatment of throat infections to avoid rheumatic fever (a cause of valve damage).
Good dental hygiene to prevent infective endocarditis.
Routine cardiac check-ups for individuals with known murmurs or congenital valve defects.

